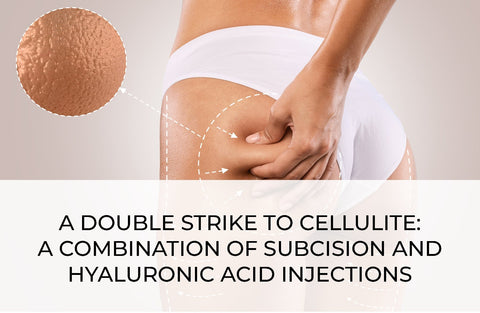
PSORIASIS AND TYPE 2 DIABETES: WHERE PATHOGENESIS AND THERAPY INTERSECT

Psoriasis is increasingly recognized as a systemic disease that extends beyond the skin and is closely intertwined with metabolic health. One of the most frequent and complex associations is the coexistence of psoriasis and type 2 diabetes mellitus (T2DM). A new review by Ouyang et al., published in Biomolecules & Biomedicine (2026), provides a detailed analysis of why these two conditions so often occur in the same patient and how understanding their shared mechanisms helps practitioners choose the right therapy [1].
Why they "meet": points of intersection in pathogenesis
The link between psoriasis and diabetes is not merely a coincidence. Research shows they share common genetic "roots" (susceptibility loci) that influence both the immune system and metabolism. A crucial concept here is gene–environment interactions, which suggests that a person's genetic predisposition (their "baseline") manifests as a disease only under the influence of external factors such as diet, lifestyle, stress, or infections. For instance, a specific gene variant may remain "silent" until a person encounters caloric excess or chronic stress, which then triggers the inflammatory cascade [2].
At the molecular level, the diseases intersect at several points:
- Systemic inflammation: Shared signaling pathways (e.g., NF-κB) and cytokines (TNF-α, IL-1β, IL-6) create a background where skin plaques and insulin resistance develop simultaneously [2].
- IL-23/Th17 axis: IL-17, a key cytokine in psoriasis, is also active in the pancreas. It can damage insulin-producing cells, linking skin inflammation to impaired glucose metabolism [3].
- Mitochondrial stress (cGAS–STING pathway): When skin or metabolic cells are under stress, their mitochondria become damaged. This triggers an ancient defense mechanism (cGAS–STING) that sharply intensifies inflammation. In patients with this "dual" diagnosis, this pathway is much more active than in those with either disease alone. In experimental models, a selective STING inhibitor reduced inflammatory cytokine levels in the skin, confirming the potential of this target [1].
- "Sugar-driven" inflammation (AGE–RAGE): In diabetes, excess blood sugar leads to the formation of advanced glycation end products (AGEs), which "cross-link" proteins and maintain persistent inflammation through specific receptors (RAGE), further impairing skin barrier functions [4].
Practical focus: how does this affect treatment?
Understanding these links changes the approach to the patient. The main takeaway for the practitioner is that treating the skin in isolation from metabolism is ineffective in such comorbid cases.
- Blood sugar control is key to dermatological success. Poorly controlled diabetes can slow the response to psoriasis therapy [1]. For example, in a retrospective study, patients with diabetes who received a half-dose of risankizumab (an IL-23 inhibitor) had lower PASI 75 response rates than patients without diabetes. In another analysis of ixekizumab (an IL-17A inhibitor), patients with diabetes achieved complete skin clearance (PASI 100) significantly later—by week 60 rather than week 12 in the control group —even after adjusting for body weight [5].
- Biologic therapy: efficacy and safety. The good news is that modern IL-17 and IL-23 inhibitors (such as ixekizumab, risankizumab, guselkumab, and bimekizumab) effectively clear plaques without worsening blood sugar or lipid levels, making them a safe choice for patients with diabetes [5]. Clinical cases have described the successful use of bimekizumab and guselkumab in patients with refractory psoriasis and diabetes, including the management of the Koebner phenomenon at insulin injection sites.
- The "dual impact" of glucose-lowering agents. Some diabetes medications have a beneficial "side effect" — they reduce skin inflammation [1]:
- Metformin — the first-line treatment for T2DM — can inhibit excessive keratinocyte proliferation and suppress inflammatory signals by activating the cellular energy sensor AMPK. In preclinical models, metformin (both systemic and topical) reduced psoriasiform skin changes in the context of diabetes. The authors also discuss the potential role of the gut microbiome in metformin's effects.
- GLP-1 receptor agonists (liraglutide, semaglutide) — popular for weight loss and glucose control — have been shown to reduce psoriasis area and severity in several studies. In a meta-analysis, liraglutide significantly lowered PASI scores and fasting blood glucose levels. In an open-label randomized trial, semaglutide combined with metformin achieved PASI 90 in nearly half of participants (6 out of 13) within 12 weeks, along with reductions in IL-6 and CRP. However, the authors emphasize that the evidence base is currently limited to small studies, and rare cases of psoriasis onset or exacerbation have been reported with GLP-1RAs, necessitating monitoring of skin symptoms.
- Pioglitazone (a thiazolidinedione) — activates the PPAR-γ pathway, suppressing NF-κB and reducing key cytokines (TNF-α, IL-6, IL-17). A meta-analysis of six RCTs showed a significant reduction in PASI scores in psoriasis patients.
- Sitagliptin (a DPP-4 inhibitor) — in an RCT, it enhanced the anti-inflammatory effect of narrow-band UVB phototherapy in patients with moderate psoriasis.
- Other approaches. In an observational study, apremilast (a PDE-4 inhibitor) not only improved PASI scores and reduced inflammatory markers (CRP, ESR) but also showed a potential glucose-lowering effect in some patients with diabetes receiving insulin or oral glucose-lowering agents.
Conclusion
Psoriasis and type 2 diabetes are two sides of the same coin of systemic inflammation. Shared mechanisms, such as the IL-23/Th17 axis, the cGAS–STING pathway, and mitochondrial stress, make them interdependent. For the practitioner, this signals that patient management must be collaborative: the skincare specialist works in tandem with the endocrinologist, and metabolic control becomes a vital tool in the quest for clear skin. The choice of therapy — whether biologics or glucose-lowering agents with anti-inflammatory potential — must account for comorbidity and associated risks [1].
References
- Ouyang L., Li Z., Zeng Y. Mechanistic insights into psoriasis and type 2 diabetes mellitus comorbidity – implications for treatment: a review. Biomol Biomed 2026. DOI: 10.17305/bb.2026.13484.
- Patrick M.T., Stuart P.E., Zhang H. et al. Causal relationship and shared genetic loci between psoriasis and type 2 diabetes through trans-disease meta-analysis. J Invest Dermatol 2021; 141(6): 1493–1502.
- Rajendran S., Quesada-Masachs E., Zilberman S. et al. IL-17 is expressed on beta and alpha cells of donors with type 1 and type 2 diabetes. J Autoimmun 2021; 123: 102708.
- Maurelli M., Gisondi P., Girolomoni G. Advanced glycation end products and psoriasis. Vaccines (Basel) 2023; 11(3): 617.
- Egeberg A., Merola J.F., Schäkel K. et al. Efficacy of ixekizumab in patients with moderate-to-severe plaque psoriasis and prediabetes or type 2 diabetes. Front Med (Lausanne) 2022; 9: 1092688.